Jan Bornschein

Contact information
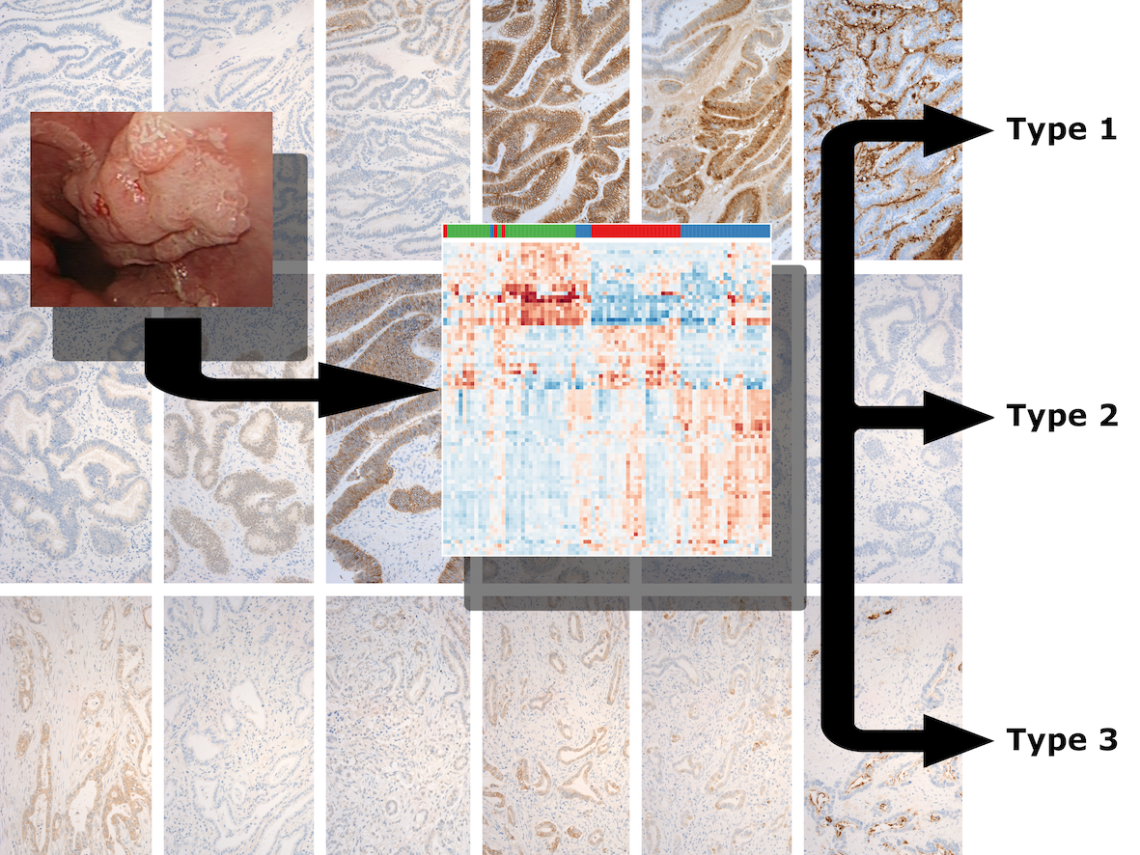
Cancer Biology
 ©
Jan Bornschein
©
Jan Bornschein
Jan Bornschein
Consultant
Jan Bornschein (MD, habil.) completed his training in General Internal Medicine and Gastroenterology at the University of Magdeburg, Germany, before joining the MRC Cancer Unit at the Hutchison/MRC Research Centre of the University of Cambridge to undertake post-doctoral research funded by a scholarship from the German Research Society. Alongside this he was appointed an Honorary Consultant at Cambridge University Hospital. From 2016 to 2017 he was interim lead of GI oncology at the University Hospital of Regensburg Germany before he took up a consultant gastroenterologist position in Oxford.
His clinical focus is directed at gastroenterology support for patients with short- and long-term side effects of cancer treatment and he is based both in Gastroenterology as well as in Oncology at OUH.
Jan’s main research interest is in inflammation-induced adenocarcinogenesis in the upper gastrointestinal tract and the impact of related risk factors. He is member of the steering committee of the German national gastric cancer guidelines and head of the working group “Epidemiology and Prevention”, and of the steering committee of the German national guideline on “Helicobacter pylori and gastroduodenal ulcer disease”.
He is committee member of the gastroduodenal section of the British Society of Gastroenterology, member of the European Society of Digestive Oncology and managing editor of Digestive Diseases.
Research Interests:
Jan Bornschein’s MD thesis addressed the effect of H. pylori induced inflammation and of reflux conditions on expression changes of transcriptions factors that are linked to premalignant conditions of the gastric mucosa. Despite focal appearance of these mucosal changes, data from this and other projects supports the hypothesis of rather a field effect that affects the whole of the stomach.
Jan’s post-doctoral research at the MRC Cancer Unit, Cambridge, focussed on the biological discrimination of adenocarcinomas of gastric and oesophageal origin at the gastro-oesophageal junction. Unbiased transcriptome analysis revealed that these cancers represent in general gastric phenotypes. Gene pathway analysis suggests different biological background of these phenotypes and makes distinct risk factor exposure likely. Sequel studies are running to look into the effect of these changes already in premalignant conditions of the stomach.
In Cambridge, he also was involved in work aiming at further characterisation of the genomic landscape of oesophageal adenocarcinoma as well as the impact of systemic chemotherapy on the mutational profile. Oesophageal adenocarcinoma is a tumour entity that presents with a very high mutational burden as well as significant copy number aberrations. Today, most patients undergo pre-operative treatment prior to surgical resection. We could demonstrate that systemic chemotherapy has no impact on the genomic landscape of these tumours in view of a systematic clonal selection process.
Current projects are focussed on the exploitation of multi-omics data integration, including single-cell sequencing, to characterise the stepwise process of gastric carcinogenesis and the interplay of these risk factors with the abundance of cell-types present in the gastric niche and the local microenvironment, including the upper GI microbiota.
Recent publications
-
Comparison of different microbiome analysis pipelines to validate their reproducibility of gastric mucosal microbiome composition.
Journal article
Lehr K. et al, (2025), mSystems
-
Screening for and surveillance of premalignant conditions of the stomach
Journal article
Luzko I. et al, (2025), Best Practice and Research: Clinical Gastroenterology
-
The road to a world-unified approach to the management of patients with gastric intestinal metaplasia: a review of current guidelines.
Journal article
Dinis-Ribeiro M. et al, (2024), Gut, 73, 1607 - 1617
-
Update S2k-Guideline Helicobacter pylori and gastroduodenal ulcer disease of the German Society of Gastroenterology, Digestive and Metabolic Diseases (DGVS).
Journal article
Fischbach W. et al, (2024), Z Gastroenterol, 62, 261 - 321
-
Liver cirrhosis is a risk-factor for Pneumocystis jirovecii associated mortality
Journal article
Peschel G. et al, (2024), Frontiers in Medicine, 11
Publications
1. Cost-effectiveness modelling of use of urea breath test for the management of Helicobacter pylori-related dyspepsia and peptic ulcer in the UK. Pritchard DM, Bornschein J, Beales I, Beresniak A, Salhi H, Malfertheiner P. BMJ Open Gastroenterol. (2021) 8(1):e000685. doi: 10.1136/bmjgast-2021-000685.
2. A Pilot Study on Automatic Three-Dimensional Quantification of Barrett's Esophagus for Risk Stratification and Therapy Monitoring. Ali S, Bailey A, Ash S, Haghighat M, Leedham SJ, Lu X, East JE, Rittscher J, Braden B; Translational Gastroenterology Unit Investigators of John Radcliffe Hospital. Gastroenterology. (2021) 8:S0016-5085(21)03087-0. doi: 10.1053/j.gastro.2021.05.059.
3. Multicentre derivation and validation of a colitis-associated colorectal cancer risk prediction web tool. Curtius K, Kabir M, Al Bakir I, Choi CHR, Hartono JL, Johnson M, East JE; Oxford IBD Cohort Study Investigators, Lindsay JO, Vega R, Thomas-Gibson S, Warusavitarne J, Wilson A, Graham TA, Hart A. Gut. (2021) 14:gutjnl-2020-323546. doi: 10.1136/gutjnl-2020-323546.
4. EGF and BMPs Govern Differentiation and Patterning in Human Gastric Glands. Wölffling S, Daddi AA, Imai-Matsushima A, Fritsche K, Goosmann C, Traulsen J, Lisle R, Schmid M, ReinesBenassar MDM, Pfannkuch L, Brinkmann V, Bornschein J, Malfertheiner P, Ordemann J, Link A, Meyer TF, Boccellato F. Gastroenterology. (2021) 3:S0016-5085(21)00733-2. doi: 10.1053/j.gastro.2021.04.062.
5. Biopsy sampling in upper gastrointestinal endoscopy - a survey from ten tertiary referral centres across Europe. Bornschein J, Tran-Nguyen T, Fernandez-Esparrach G, Ash S, Balaguer F, BirdLieberman E, Córdova H, Dzerve Z, Fassan M, Leja M, Lyutakov I, Middelburg T, Moreira L, Nakov R, Nieuwenburg SAV, O'Connor A, Realdon S, DeSchepper H, Smet A, Spaander MCW, Tolmanis I, Urbonas T, Weigt J, Hold GL, Link A, Kupcinskas J. on behalf of ENIGMA Dig Dis. (2020) doi: 10.1159/000511867.
6. A dynamic CD2-rich compartment at the outer edge of the immunological synapse boosts and integrates signals. Demetriou P, Abu-Shah E, Valvo S, McCuaig S, Mayya V, Kvalvaag A, Starkey T, Korobchevskaya K, Lee LYW, Friedrich M, Mann E, Kutuzov MA, Morotti M, Wietek N, Rada H, Yusuf S, Afrose J, Siokis A; Oxford IBD Cohort Investigators, Meyer-Hermann M, Ahmed AA, Depoil D, Dustin ML. Nat Immunol. (2020) 21(10):1232-1243. doi: 10.1038/s41590-020-0770-x.
7. Cytosponge-trefoil factor 3 versus usual care to identify Barrett's oesophagus in a primary care setting: a multicentre, pragmatic, randomised controlled trial. Fitzgerald RC, di Pietro M, O'Donovan M, Maroni R, Muldrew B, Debiram-Beecham I, Gehrung M, Offman J, Tripathi M, Smith SG, Aigret B, Walter FM, Rubin G; BEST3 Trial team (local PI Oxford), Sasieni P. Lancet. (2020) 1;396(10247):333-344. doi: 10.1016/S0140-6736(20)31099-0.

